MR-Guided Focused Ultrasound (MRgFUS)
Incisionless Treatment for Tremor Disorders
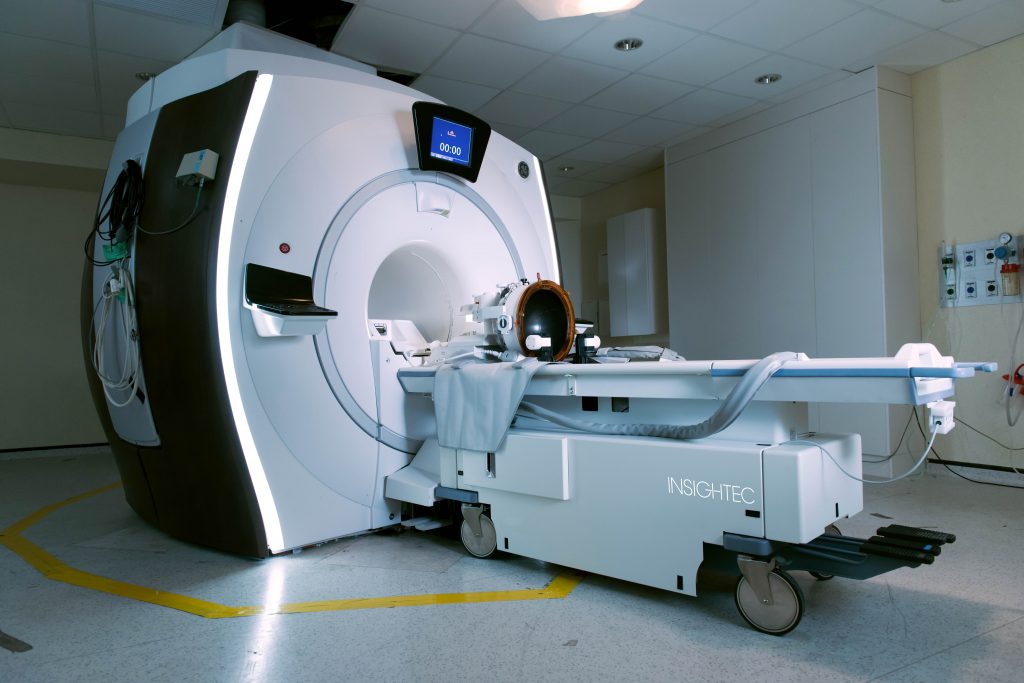
MR-guided focused ultrasound (MRgFUS) is an advanced, non-invasive treatment used for patients with essential tremor and tremor-dominant Parkinson’s disease.
It combines high-intensity focused ultrasound energy with real-time MRI guidance to precisely target and treat small areas deep within the brain, without the need for surgical incisions, implants, or radiation. This technology represents a shift from conventional neurosurgery toward image-guided, incisionless therapy.
Conditions Treated
MRgFUS is currently used in carefully selected patients with:
- Essential tremor that is not adequately controlled with medications
- Parkinson’s disease with significant tremor symptoms
- Other indications may be considered based on specialist evaluation
Patients are typically referred when symptoms interfere with daily function such as eating, writing, or self-care.
How the Technology Works
MRgFUS works on a fundamental principle of energy convergence.
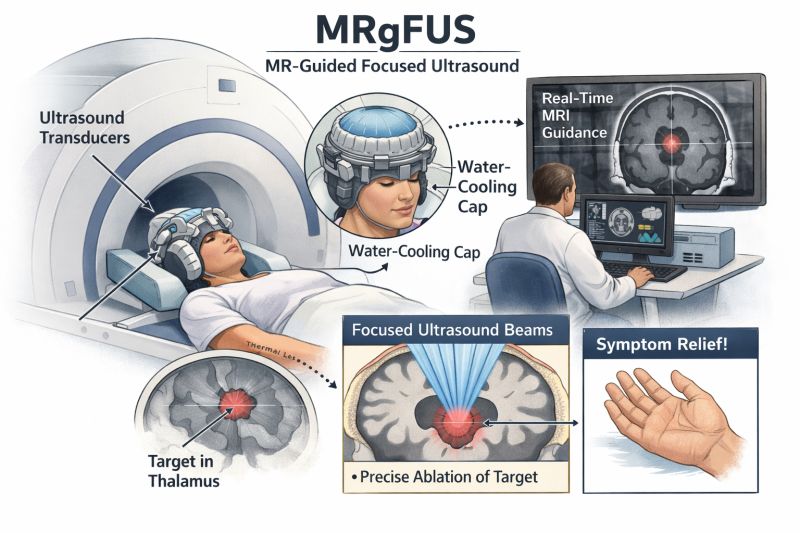
1. Focused Ultrasound Energy
Multiple ultrasound beams are generated from a transducer helmet placed around the patient’s head.
Each individual beam passes safely through the skull and brain tissue without causing damage.
However, when these beams converge at a single, predefined target, they collectively generate sufficient energy to produce a controlled thermal effect.
2. Precise Thermal Lesioning
At the focal point, the temperature rises (typically 55-60°C), creating a small, controlled lesion in the target area of the brain.
For tremor, this target is usually within the thalamus (VIM nucleus), a region involved in abnormal tremor circuits.
This interruption in neural signaling leads to reduction in tremor symptoms.
3. Real-Time MRI Guidance
MRI plays a critical role in three ways:
- Targeting: Identifies the exact anatomical location
- Thermometry: Monitors temperature changes in real time
- Feedback: Confirms accuracy and safety during treatment
This allows the treating team to make incremental, controlled adjustments, ensuring precision while minimizing risk to surrounding tissue.
4. Intra-Procedural Clinical Testing
Unlike most procedures, MRgFUS is performed with the patient awake.
This allows:
- Real-time assessment of tremor improvement
- Immediate feedback from the patient
- Fine-tuning of treatment before final lesioning
Why this approach is different
Traditional neurosurgical options such as Deep Brain Stimulation (DBS) involve:

- Surgical implantation of electrodes
- Hardware placement inside the body
- Multiple stages (surgery + programming)
In contrast, MRgFUS:
- Requires no incision or hardware implantation
- Is performed in a single session
- Provides immediate clinical feedback
However, unlike DBS, MRgFUS creates a permanent lesion and is not adjustable after treatment, which is an important consideration during patient selection.
What to expect during treatment
Before the Procedure
- Clinical evaluation by movement disorder specialists
- MRI and imaging-based planning
- Assessment of suitability
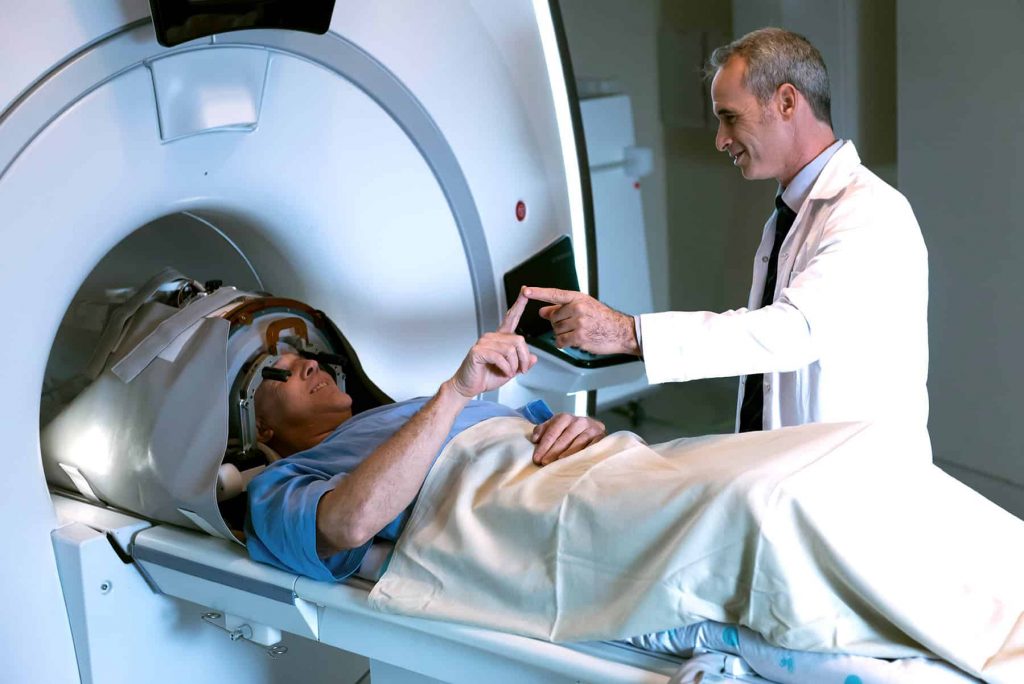
During the Procedure
- The patient lies inside an MRI scanner
- A specialized ultrasound helmet is fitted
- Low-energy test sonications are performed initially
- Gradual increase in energy to achieve therapeutic effect
- Continuous MRI monitoring and clinical assessment
Total duration: approximately 3-4 hours
After the Procedure
- Observation for a short period
- Most patients are discharged the same day or next day
- Follow-up evaluation for clinical outcomes
Benefits
- Non-invasive (no incision or craniotomy)
- No implanted devices
- Reduced risk of infection and surgical complications
- Short hospital stay
- Rapid recovery
- Immediate intra-procedural assessment of effectiveness
Limitations and Considerations
- Typically performed on one side of the brain (unilateral)
- Effects are permanent and not adjustable
- Not all patients are suitable candidates (e.g., skull density factors)
- Requires careful selection and counseling
Safety
MRgFUS is performed under continuous MRI guidance with real-time thermometry, allowing:
- Controlled energy delivery
- Monitoring of adjacent structures
- Immediate detection of off-target effects
Reported complications are generally low when performed at experienced centers
Care at
Christian Medical College Vellore
Patients are evaluated and managed through a multidisciplinary team, including:
- Movement disorder neurologists
- Functional neurosurgeons
- Neuroradiologists
- Specialized nursing and rehabilitation teams
The program is integrated within the Department of Neurological Sciences, ensuring comprehensive care from evaluation to follow-up.
Meet the Team
Care is provided by specialists in movement disorders at Christian Medical College Vellore
Movement Disorders Neurology
- Dr. Shaikh Atif Iqbal Ahmed, D.M (Neurology)
Referral and Appointments
Patients can be referred for evaluation through:
- Neurology / Movement Disorders Clinic
- Direct consultation appointments